
This post is all about healing ulcerative colitis and Crohn’s disease flare-ups.
If you’re currently in the midst of a UC flare-up, this article is for you.
I’ve written this post to give you as much information and as many options as possible to deal with an ulcerative colitis flare-up.
This is information you won’t read anywhere else.
Its hard-earned knowledge learned on my own healing journey and my work with others since 2008.
Not everything I talk about here is for everyone, but these are the things that I’ve seen empirically work.
There’s something here that will help you.
You’re not alone and you can live a life that’s different from the one you’re currently living.
Avoiding an Ulcerative Colitis Flare-Up to Begin with – Systems Not Symptoms
I can still remember many years of living in fear of the next flare-up.
It’s a constant worry when you have UC.
Flare-ups become this constant, nagging fear. (Am I right? Let me know in the comments!)
Always looking for signs of blood in the toilet.
That sinking feeling when things are looking worse, you’re going more and it’s more urgent.
When you know it’s not going to slow down and you’re in trouble.
Always afraid the next meal will set the UC off again.
Here’s the thing – we have to think in terms of systems not symptoms.
Flare-ups are actually starting weeks or months before we become aware of them.
Have you ever noticed that your UC or Crohn’s seems to get worse “at the worst possible time?”
When stress is at a peak in your life?
I used to always feel like my body was letting me down.
In truth it was the other way around – I was letting my body down.
If you oscillate between periods where your UC is calm and periods where it flares-up, that means some things you’re doing are helping and some are causing problems.
Almost certainly, the better times involve better eating, better sleep and less stress.
The times when the UC isn’t doing so well are usually preceded by a pattern of dietary transgressions, high-stress, lower self-care and no downtime.
When you learn the patterns and learn to control and heal ulcerative colitis flare-ups on your own, you take control of your life back.
You can learn to eat and think and live in ways that move you toward health.
Ulcerative Colitis Flare-Ups are Caused by Diet and Stress
The cause of an ulcerative colitis flare up will be many interconnected things. But they will generally fall into two categories: Food and Stress.
Eat Meat, Vegetables and Fruit
That’s really about it. That’s my baseline diet. Meat, vegetables and fruit.
I don’t really eat much else.
Foods that will generally trigger the immune system and an ulcerative colitis flare-up are:
- Eggs
- Dairy
- Grains (even gluten-free)
- Nuts and Seeds
- Nightshade Vegetables (Tomatoes, Peppers, Eggplant)
The effects of these foods are not necessarily immediate.
I went down the raw and fermented dairy rabbit hole years ago and spent a lot of time thinking I was benefiting from the probiotics and raw, undenatured proteins and fats.
But sooner or later I’d always get into a flare-up.
Remove the dairy, heal. Reintroduce the dairy, flare up.
Wash, rinse, repeat.
Eggs were the same. They’d seem to be working for a while, but then my immune system would start to get more active and UC symptoms would manifest sooner or later.
Paleo Autoimmune Protocol Diet (Paleo-AIP) – Remove Immune System Triggers
After many, many years, I’ve reached the point where I just don’t eat anything I shouldn’t.
I’ve found over the last 17 years on my healing journey with UC that maintaining an absolutely strict, individualized Paleo Autoimmune Protocol diet (Paleo-AIP) is the way to go for healing UC and staying out of flare-ups to begin with.
I eat what I eat and I don’t deal with flare-ups or UC symptoms anymore.
I’m not going to make a big case for diet in general or Paleo-AIP specifically here.
Everything you need to go deep on diet for UC and Crohn’s is here in these posts:
Ulcerative Colitis and Diet – Effective Eating Strategies and Food Choices for Healing
Eating for Ulcerative Colitis – with My Personal Meal Examples
Skip the Reintroduction Phase
There really isn’t a “reintroduction” phase with Paleo-AIP, in my opinion.
At least not for ulcerative colitis and Crohn’s.
Not for any serious, chronic, autoimmune illness.
When you start to “reintroduce” foods you will generally see a flare-up sooner or later.
An absolutely strict, lifetime Paleo-AIP diet is a major key to healing UC and staying out of flare-ups.
Diet Screw-Ups are a Major Cause of Flare Ups
It’s almost cliché for me now, where I run into someone at the dispensary who has UC or Crohn’s and they’re “having a flare up.”
Upon further investigation there was some kind of Super Bowl party or a birthday or a vacation or something that moved their diet from simply “somewhat OK” to “off the rails” and in a few days or a few weeks, a flare-up developed.
This is a self-inflicted flare up.

And the marijuana-infused brownies and cookies won’t help this flare-up either. It’s a myth that marijuana-infused junk food will do anything for anyone in terms of healing an ulcerative colitis flare-up.
These are the patterns to begin noticing.
When do symptoms increase or manifest and what was going on in the days and weeks leading up to it?
We all have food and lifestyle triggers for UC and knowing what yours are is going to make a big difference for you.
Stress and Inflammatory Bowel Disease Flare Ups
We get just a certain number of “units” of stress or stress tolerance per day. This is total stress.
Everything adds up.
You don’t have 100 stress units for workouts, another 100 for your relationship, a third 100 for your career.
It’s all coming from a single place and it can be overwhelmed by life pretty fast.
This is particularly true when we’re already operating at near-capacity as a general way of existing.
Further, UC and Crohn’s put a huge energy burden on the body.
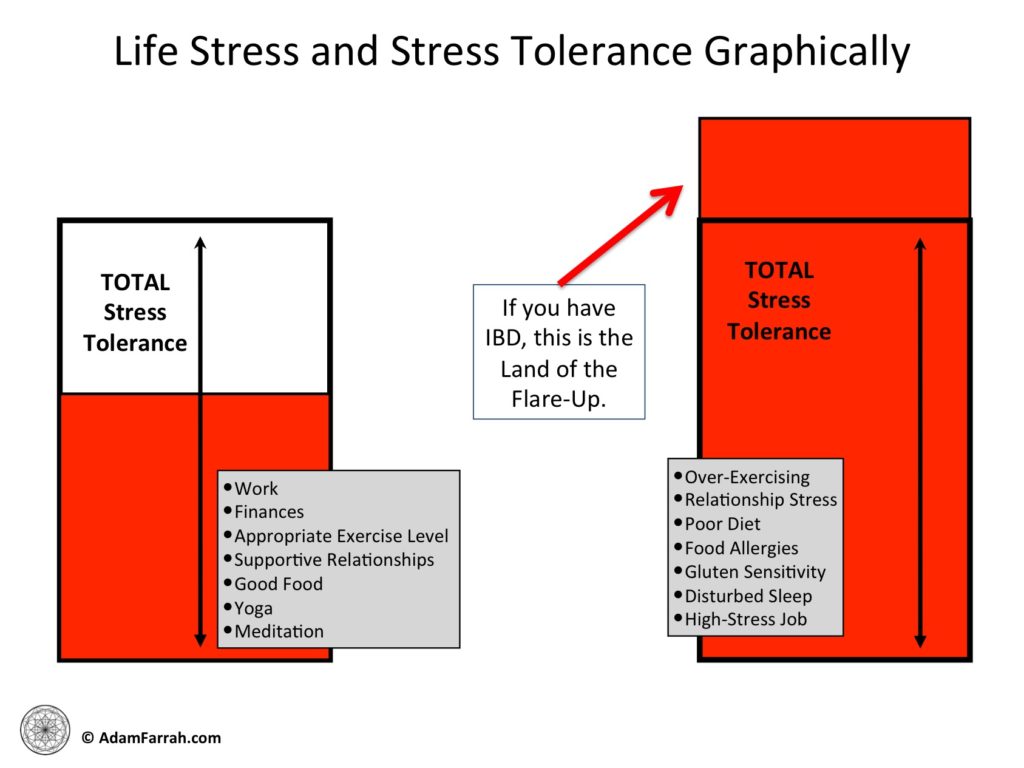
Above, in Figure 2, is the graphical representation of stress tolerance with appropriate life stress on the left and overwhelming life stress on the right.
This is also why some foods affect us sometimes and not others – you’ll tolerate some foods better when you’re less stressed and well-rested.
I sometimes have trouble with even the best food when stress is too high.
This happens a lot less lately because I’ve learned how to keep my stress under control with yoga and meditation.
Stop Medicating Ulcerative Colitis Symptoms and Ignoring Root Causes
If you look at the commercials for the current crop of UC and Crohn’s disease meds, you can see it’s all about continuing to eat what you’re used to eating and continuing to live your old life.
That’s the “benefit” of the pharmaceutical product from a marketing standpoint.
You can have your life back and go back to doing what you like to do and be free of ulcerative colitis.
The idea is: Don’t look at your behavior or modify anything for your health, just take a pill and keep going. Or an infusion in this case.
The entire premise of the above commercial is that IBD is negatively affecting this guy’s life and his life with his family. He wants to be free to live how he lived before he got sick.
This even includes eating cupcakes and ice cream with his child.
But how we lived before we got sick is a big part of what made us sick to begin with.
One of the ultimate truths I’ve learned about healing UC – and chronic illness in general – is this:
If you want to change your life, the way you’re living has to change.”
– Adam Farrah
Slow the F*ck Down Already
This used to be me. The blonde actress at the start is going into a conference room for a stressful meeting with her boss at work. While struggling with Crohn’s.
I excused myself from plenty of important meetings to go shit blood in my early UC years. I even had a phone interview for a job once while sitting on the toilet.
The other guy in the commercial is traveling and catching planes in an airport. With ulcerative colitis.
Look, I get it. Ulcerative colitis sucks and so does changing your life and “missing out” on things and foods and events and the like.
But you need a period where you slow down, focus 100% on diet and health and let yourself relax and heal – on your body’s timeline, not your ego’s.
Some people may need to change jobs or end relationships to finally heal.
I certainly had to.
I would have healed years sooner if I had let go of things and people and practices and habits that didn’t serve me sooner.
If your life has you chronically running and stressed and exhausted, that is a major cause of the recurring problems you’re having with IBD.
If you are one of these people with UC or Crohn’s and you’re chronically exhausted and stressed and running and taking care of people or solving problems, definitely investigate Codependency.
You can learn everything you need about Codependency as it relates to UC in my post Ulcerative Colitis, Codependency and Interpersonal Boundaries – Psychological and Spiritual Factors in Inflammatory Bowel Disease
Healing an Ulcerative Colitis Flare-Up
Warning and Disclaimer
UC is a very dangerous, aggressive and devastating disease.
Flare-ups are no joke and can get out of control very quickly. Don’t mess around with them or take them lightly.
I teetered on the edge of death for a few years starting in 2004. Before I knew enough to move myself out of that space and onto the road to health.
I made a bunch of trips to the ER in those early years.
You must realize that this is a very serious disease and you can get into trouble with it.
Proceed at your own risk with anything you learn here.
If you’re in a serious flare-up and can’t get it under control, get to a doctor or hospital.
That said, here are the methods I’ve used – natural and otherwise – to get a flare-up under control over the years.
Fasting to Control and Heal Ulcerative Colitis and Crohn’s Disease Flare Ups
I did a lot of fasting in the early days when I was very sick.
I fasted for over a week on just water several times.
Fasting for a day or few can be a really effective way to shut down a flare-up. I used to do this all the time.
Giving your digestive tract a day or two off can really give it a chance to heal. Your digestive lining heals quickly. A short break can make a big difference.
Not eating also means you’ll go to the bathroom less.
Sometimes I would fast just to avoid having to use the bathroom for a trip or event. Just empty myself out and not have to worry about it.
I’d sit at dinner and drink water while everyone ate. Get ready for the social pressure when you do that one…
Fasting Generally is Safe
People can get really, really freaked out about fasting. Like if you go a few hours without eating you’ll die or something. It’s crazy.
Our genes have millions of years of survival mechanisms built in to keep us alive in times of little food or famine.
Because we’re so used to eating all the time in this ridiculous modern world, it seems like not eating for 24 or 36 hours is like this big scary thing.
It’s not.
In my own case years ago, I was so sick and inflamed eating made me feel terrible. Hungry as I was, not eating felt better than eating most anything.
Fasting is quite safe, particularly in very short doses of a day or two.
Just take it easy. You will be tired and light-headed sometimes. This is something to try over a few days that you have to yourself where you can take it slow and easy.
Ulcerative Colitis Flare-Ups, Smoothies and a Liquid Diet
Fruit and water smoothies have always been tools in my flare-up healing arsenal.
You may be hungry during a flare-up, but your ability to digest much of anything is severely compromised.
If fasting on just water is more than you can handle, fasting on just banana and water smoothies can be really effective.
I Still Use Smoothies and Smoothies Fasts Today

This particular smoothie recipe has been a daily staple for me for many years now:
- Nutiva Hemp Protein Powder
- Fresh bananas
- Fresh fruit like mangoes, strawberries or blueberries
- Organic coconut oil
- Organic India Psyllium Husk Fiber
- Celtic Sea Salt
- Water
Warning: The psyllium husk fiber is not a good idea during a flare-up!
Psyllium is just too irritating. You need to be more healed before starting in on that.
I also recommend holding off on the hemp protein during a UC flare up as well.
This combination of “stuff” blended together is about as close as I’ve found to foods that are actively healing for the gut and UC.
This shake daily makes a HUGE difference in my bowel health and stools. I’ve been told the same thing by others – with and without UC – who have used the recipe with consistency as well.
Every so often, I eat nothing but smoothies for a day.
It gives my digestion a break and I always come back stronger.
Smoothies are easy to digest and, when done right, will firm up and bulk up a loose stool like nothing else.
Watch Out for Emotional Eating, Binging and Self-Sabotage
Flare-ups can drive certain negative behaviors that make the flare-up worse.
We’re strange creatures, humans.
Emotional Eating and Binging
In the very early days, flare-ups would sometimes drive more poor food decisions with me.
Some of this comes from “self-nurturance” when sick. Most of us are conditioned to eat comfort food when scared or sick. Or both.
Sometimes the emotions that come up during an ulcerative colitis or Crohn’s flare-up are so painful, emotional eating starts up.
This is also problematic because we’re hungry and it’s hard to make good decisions around food when we’re starving.
When I first got sick in 2004, I remember watching Food Network all the time. I became obsessed with food. I’ve heard this from others too.
And don’t have tempting stuff in the house if you can help it.
Other than that, just commit to taking care of your health and putting healing ahead of momentary pleasure or emotional eating.
Self-Sabotage and Apathy
Everyone engages in self-sabotage sooner or later.
Self-sabotage and apathy are another duo I struggled with very early on.
I’d do these crazy strict diets that didn’t totally work, get into a flare-up and get so discouraged that I’d break the diet and just eat something “good.”
When we try a new diet for UC and end up in a flare-up eventually, the “diet has nothing to do with it” myth seems like it might not be such a stupid statement after all.
Now, anything goes.
Don’t fall into this.
You can eat and live in ways that heal UC and Crohn’s.
“Diet has nothing to do with ulcerative colitis and Crohn’s disease” is Myth #1 in my blog post The 14 Myths About Healing Ulcerative Colitis.
Curious what the other 13 myths of healing IBD are? Check out the post!
Using Medical Marijuana to Heal an Ulcerative Colitis Flare-Up

I always tell my clients who are in a flare-up and able to use marijuana to use as much as they can stand.
I’ve also encouraged clients in states that allow medical marijuana to get a card and get to using medical marijuana for their UC or Crohn’s.
Medical marijuana was a complete game-changer for me. It took me the rest of the way in my healing.
Want to learn all about medical marijuana for ulcerative colitis? Check out my epic post Medical Marijuana for Ulcerative Colitis – The Principal Guide.
Increase Dosage
I’ve healed minor flare-ups with marijuana within 24-48 hours over the years.
I’ve yet to find a “too much” when I’m using medical marijuana to heal an ulcerative colitis flare-up or ulcerative colitis in general.
The point is, if you’re sick and flaring, you need to get it under control fast.
High-dose THC is an exceptional anti-inflammatory and a very good way to control a flare-up.
Get as much THC as you can stand if you’re trying to heal a flare-up.
Over-the-Counter CBD for Flare-Ups
If you can’t get marijuana at all, or you’re in a state with a low-THC mandate in their program (eye roll), high-CBD medical marijuana products and even over-the-counter CBD supplements can be a good option.
Here’s an entire post on all things CBD: High-CBD Medical Marijuana – The Principal Guide [LINK]
The above post will give you a strong overview of CBD, CBD supplements and cannabinoid chemistry.
CBD Dosage for a Flare-Up
Anecdotally, I’ve been seeing good results from CBD in clients in the 50-100mg range three times a day. Your results may vary, but that’s where I’ve seen results empirically.
I have seen clients do well on over-the-counter CBD when medical marijuana isn’t available in their location.
Are you currently using CBD to control a flare-up with good results? What kind of dosage has been working for you? Let us know in the comments!
Prednisone Can Shut Down a Flare-Up Fast
The last time I took anything for UC was in 2009. That’s the last flare-up that I needed prednisone for.
Since then, food, lifestyle changes and medical marijuana have me free of flare-ups for many years now. [LINKS]
Back in the olden days, when I was really sick with UC, there was no Humira or Entyvio.
All they really had was prednisone and Asocol or another mesalamine drug.
None of the mesalamines did anything for me. The majority of people with UC I speak to say the same.
And the prednisone made me mentally nuts.
More nuts.
But short cycles of prednisone can shut down a flare-up pretty quickly without a lot of side effects.
If you have a decent GI doctor, you can discuss a short cycle of prednisone instead of a biologic or lifetime of high-dose prednisone.
I’m not against pharmaceutical intervention. I’m just against medicating symptoms perpetually and not addressing the root causes.
A short course of prednisone under a doctor’s supervision might be what you need to heal the flare-up and set yourself up to rebuild your lifestyle and avoid another UC flare.
This gives you the benefit of a powerful pharmaceutical without the long-term commitment of a lifetime biologic or (gasp) lifelong prednisone.
It’s Between You and Your GI Doctor
What you decide to do and how you decide to use prednisone, if you decide to use it, is up to you and your doctor.
I discuss my results with prednisone – from back when prednisone was about all there was to treat UC – because I think it’s an effective short-term solution that can heal a flare-up pretty fast. And some doctors do still prescribe it pretty routinely for UC.
Prednisone can get you back on track when nothing else is working.
Prednisone is a Steroid, Use it Like One
I spent many years in the bodybuilding world. Prednisone is a catabolic steroid, as opposed to the anabolic steroids that bodybuilders use.
Bodybuilders cycle steroids so they remain effective and side-effects are kept as low as possible.
When I got into trouble with a flare-up in years past, I’d go high on the prednisone and then taper it down and get off it. Just like a bodybuilder on anabolic steroids.
The original GI doctor I had in 2004 wanted me on high-dose prednisone for life.
A lifetime of prednisone would have wrecked my mind and body and I knew there was no way I could take a powerful, high side-effect drug like that indefinitely.
If you’re currently in a flare-up and have a good GI doc that you can work with, discuss a short course of prednisone, maybe a month or two.
You might start high (40-60mg) and stay there for a week or two and then taper it down over a few weeks and get off it.
I did the above about 10 times over the years when I was still really bad with UC.
I had a sympathetic and somewhat modern-thinking primary care physician who helped me and wrote the prescriptions for the prednisone. They are out there. You just have to look and leave the doctors you don’t resonate with.
Exercise and Ulcerative Colitis Flare-Ups
We exercise way too intensely in our culture generally.
This is even more the case for people with an autoimmune disease.
I remember one woman with UC who was a marathon runner. She got a treadmill so, during flare-ups, she could run indoors next to the bathroom and jump off the treadmill to use the toilet during the workout.
Because bloody diarrhea is even more fun with your heart rate pounding and your body dripping with sweat.
This is all very “smart” and “UC isn’t going to stop me” and all. Admirable in the West. No excuses. Hustle. Powering through no matter what.
The problem is, particularly with an activity like long-duration running, the body just sees it as another stress to deal with.
The treadmill woman later ended up with a full colectomy. Coincidence?
The outcomes for UC are abysmal if you don’t get it under control and keep it that way.
The problem is, this kind of pushing and pounding and hard exercise on an already abused and exhausted body is just going to keep the flare up going.
It’s more inflammation and more damage for the body to deal with.
If your body is so sick and messed up it’s in a UC flare-up, what the hell kind of athletic and training progress do you think you can make in that condition?
I generally recommend gentle, restorative yoga as exercise during a flare-up.
The body’s ability to deal with stress is already overwhelmed when we have UC in general and during a flare-up in particular. To continue with a high-cortisol, depleting activity like running is just digging the hole deeper.
Intense exercise further increases inflammation. The body is already over-inflamed and struggling from IBD.
Benefits of Exercise for UC
These are some of the basic benefits of exercise for UC. Some are obvious, some aren’t.
Cortisol and Stress Management
The hormonal profile we have when our life habits include consistent and appropriate exercise is entirely different from that of a sedentary person.
Proper exercise results in a cascade of beneficial and healing hormones. This cascade moves us toward a “rest, digest and repair” state. This is the opposite process to an inflamed and stressed-out, cortisol-based hormonal state.
Improved Sleep Quality
Within a few weeks of beginning a sensible and appropriate exercise program, sleep quality markedly improves.
Massage Internal Organs
Certain types of movement can be very healing to the internal organs. Yoga is a major one for this benefit. (Check out my recent blog post: Do Yoga and Meditation Heal Ulcerative Colitis and Crohn’s Disease?)
The movement and abdominal contractions massage the internal organs and moves them around a bit.
Improved Self-Esteem and Sense of Well-Being
Ulcerative Colitis will really take a toll on your self-esteem. One of the best ways to build that self-esteem back is with regular, intelligent and productive exercise.
Completing workouts and investing in yourself and your health will dramatically change your self-concept and increase your self-esteem, self-confidence and feelings of well-being.
Negatives of the Wrong Types of Exercise for UC
There are a number of negatives and downsides associated with the wrong types of exercise when it comes to ulcerative colitis.
Increased Inflammation and Cortisol
With UC, the body is already inflamed, unhappy and out of control. More inflammation from exercise, combined with exercise-induced systemic stress, can create a number of problems – including a flare-up.
The wrong kinds of exercise overwhelm the immune system and a flare-up can break through the weakened defenses and manifest.
Joint Pain and Injuries
Autoimmune illness and joint pain go together. Exercise of the wrong type, along with improper exercise form, further degrade joints and inflame muscles.
A body struggling with UC is more injury prone when exercising because of systemic inflammation.
Systemic Fatigue
Exercise puts tremendous stress on the body and immune system.
Ulcerative Colitis also puts tremendous stress on the body and immune system.
The combination of UC and exercise can be overwhelming and trigger a flare-up or even additional autoimmune symptoms.
This is further aggravated when training is too frequent, improper or too intense.
Yoga and Meditation
As I mentioned above, I recommend gentle, restorative yoga as the primary mode of exercise during a flare up.
I add meditation in here because meditating after yoga is the perfect time and yoga and meditation complement each other and act synergistically together.
Yoga and meditation are particularly helpful in healing ulcerative colitis and Crohn’s disease.
Conclusion
Systems Not Symptoms.
The world is changing quickly.
The way people live and work is changing.
There’s no better time to reinvent yourself and your life and move beyond UC.
But trying to “manage a flare-up” once it’s already underway is the hard way.
Build a life that takes you toward health.
Build the systems and habits in your life so doing what keeps you healthy is easy and automatic.
Want to learn about the higher-level lifestyle changes required to heal UC and Crohn’s?
Check out my blog post: Healing Ulcerative Colitis with Conscious Lifestyle Changes and Practices.
I’ve given a lot of information here. Not everything is for everyone, but there’s a lot here for anyone with UC.
Get the flare-up under control and get yourself out of danger.
Then, build a diet and lifestyle that takes you toward health. And add some medical marijuana if you can. And some over-the-counter CBD if you can’t.
Good luck.
Was this post helpful? Did I miss something you’d like to see me include? Let me know in the comments!
Wow Adam…thank you so much…this makes so much sense to me…I am not crazy, there is other ways!
I was diagnosed in the 1990’s with ulcerative colitus and witnessed my mother diagnosed with Crohns have her life taken away from her since her 40 s and see her body crumble, bones breaking, on opiates and steroids and more meds for other health issues until she passed in her 80s, she had no quality of life even with the ton of pills she was taking.
I was told to never expect to heal, it’s chronic and I would have to take pills my whole life by my GI and maybe someday wear a bag, I was 29. The pharma treatments were saved my life but not giving me a quality of life, I had awful side affects.
I took another route, I haven’t taken prednisone since 1993. Once in remission, i started smoking cigarettes again after reading some research on the effect of nicotine ( was smoke free for 9 years prior and proud of it but it was better than steroids for life) and continued a spiritual and wellness journey on steroids lol ( not the meds), lol . I remained symptoms free for over 25 years….never found the gutts to stop smoking until I could really slow down.
When I retired from teaching in the public school system, mother passed away and I stopped smoking cigarettes and got mild flareup, so started 5 cigs a day again and added smoking cannabis for pain, which has been an on and off habit in my life since the 70s, i am not much of a drinker. I went into remission and quit smoking cigs again.
Then after a year of smoking one joint a day and feeling guilty about it, I quit and flared up real bad after a week while going into covid lockdown. I was in big trouble this time!
Creation/God guided me, …I did not want to smoke cigarette anymore, I was guided back to cannabis ( smoking and tincture) and took as much as I could bare cause i was deterioting fast and God willing, I recovered at home.
You have confirmed that I did Good by Me! Thank you!
Today, I am well and grateful! And after reading You, i am even more proud of myself for listening to my hearts of hearts through all those years! My way was not mainstream but I am today still alive and kicking with hope! This is almost like writting a life revue! Well done, Danie!
I have to admit that I was pissed that I still needed plant medecine after all the therapy through the years, all the life changes I had made with food, less stress, retired now with real time for me, meditation every day, regular energy and physical care, psychotherapy, journeying, exercice….etc.
Patience and Acceptance is the menu du jour!
I was hoping I would be free of it completely…so i have been asking God/dess for some clarification…so hard on myself, right? A masterpiece in progress!
The Beloved Universe responds…. I found you Adam. And yes I do smoke pot ( healing old uneducated propaganda about cannabis, it is medecine! ) and take cbd tinctures, they are part of my supplement regimen, it is legal in my country and
]
Wellness is my passion, making sense of the challenges that my soul has chosen to live on this Earth is my way of navigating life. This is me!
I hope some day to not have to smoke to give my lungs a break, I have just recently found a local source of a full spectrum tincture and feeling good about it, and cultivating my confidence to stop smoking some day. You are helping me cultivate this confidence that I will be fine and if I need to be challenged again I will find my way back to health. I can do this , I have and i will again if I need to, to grow. It is time for me to starts being proud of myself, loving this body even when it scream loud….I know now how to listen to myself and find the ressources i need. Hope!
The pharmaceuticals were limited in the 90s, and prednisone ( it saved my life a few times and the life of my baby, I am grateful), but it was becoming my best friend and i wasn’t in my right mind during and the 6 months off, then another flare up, i had aweful side affects physically and emotionally and I decided to take another route …I was told I was woo woo to think I could ever heal. I am not that crazy am I? And Here, you are dear Adam sharing your story, helping me find peace about my own journey and my mother’s.
My relationship with her was abusive at times, opiates and steroids etc messed up her body and her mind; one day, nice, the next, a raging lunatic ( I was also like that on steroids, like peri menopause, what an emotional roller coaster)…today you have helped me go even deeper with forgiveness…I am so grateful! I am reminded that she couldn’t help it, it wasn’t personnal, her body was breaking apart, she had little relief!
So from the deepest part of my heart and soul, thank you!
I am not alone, there are other ways! I was guided, my self esteem is stronger, I can trust this body and my soul to show me the way!
Blessed Be Adam and Namaste💞
Danie
Hey Danie,
Yeah, the road is hard with the pharmaceuticals. That was always my biggest fear. A terrible quality of life.
Happy things are better for you, the cannabis is working and you found the blog! Keep in touch!
Adam